By Moez Zeiton.
Tripoli, 26 June:
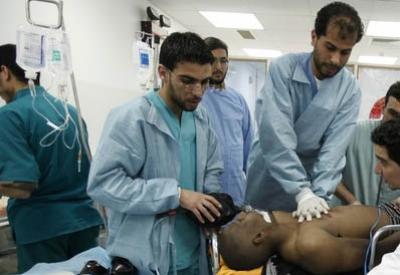
The devastation left in the wake of the past year’s events has seen many unprecedented challenges for . . .[restrict]Libya’s leaders. The causes and effects of conflict on security, leadership, corruption, ethnic divisions and the extractive industries have all been documented in the mainstream press. Much less, however, has been said about the impact on the ‘softer’ sectors of health, education and social welfare.
Pre-revolution health
Prior to the revolution, Libya was often lauded as having the highest Human Development Index (HDI) in Africa. The discovery of oil and natural gas in the late 1950s transformed the country from one of the world’s poorest, dependent on foreign aid, into one of the richest in the region. Due to its modest population of approximately six million people, Libya was, on a per capita basis – at least on paper – the third richest country in Africa.
Since the discovery of its hydrocarbon wealth, Libya has shown continual progress in health indicators, with its main achievements being near universal coverage in its childhood immunisation programme and its achievement of close to 100 per cent rate of attended births in hospital. According to World Health Organisation (WHO) figures, Libya also leads the way in having the highest number of hospital beds per capita in the region.
All that glitters is not gold…
For all of these achievements, the truth of Libya’s healthcare situation requires a closer analysis. Increasing globalisation, education and the realisation of broad public health interventions (such as safe drinking water and sanitation) are the main contributors to the aforementioned achievements. However, while looking at health indicators over the past 10 to 15 years, quite a different picture of the state of Libya’s healthcare emerges.
One of the most significant public health issues in Libya is road traffic accidents. This has seen mortality figures double over the past 15 years and is currently the third highest cause of death in Libya, leaving many more with permanent disability.
Furthermore, on closer inspection of hospital bed figures it emerges that a significant number of hospitals have undergone long periods of construction or renovation, some lasting as long as eight or nine years, while others remain incomplete (as is the case in Misrata and Sebha), meaning that many of these beds are not actually in use or are of poor quality.
Whilst all Libyan citizens have enjoyed an all-encompassing healthcare package that was technically free at the point of use, there has been concern about the quality of services provided. This, coupled with a widespread distrust of public facilities, has meant that a multi-million dollar medical tourism industry has emerged in neighbouring countries solely to cater for Libyan patients. Accordingly, out of pocket expenditure on healthcare is likely to be significantly higher than those stated in official government figures of 12 percent – the World Health Organisation (WHO) estimates the figure to be closer to 20%.
Emblematic of the poor management and allocation of resources under the Qaddafi regime was the procurement by the Libyan Ministry of Health some years ago of a positron emission tomography (PET) scanner – a medical research and diagnostic tool used mainly in the field of oncology. The grand opening for the multi-million dollar PET scanner was broadcast on Libyan state television to much fanfare but since that day, the PET scanner has remained locked in a room unused due to a lack of technical expertise to operate the machine.
Prior to the start of the uprising against Qaddafi in February 2011, Libya was already struggling to define a clear strategy in the health sector and the events of the Libyan uprising have further confounded these efforts.
Looking for leadership
Libya’s new Ministry of Health has sought the help of WHO in order to revitalise the country’s “shattered health system” but the country’s unstable political climate has made substantive progress difficult and slow.
The revolution took a heavy toll on Libya’s people. Although there are no accurate figures for the numbers of people killed, missing or injured, estimates are usually in the tens of thousands. Many patients (either individually on their own expense or through various initiatives under local and national authorities) were sent abroad for treatment. The processes for sending patients abroad were far from transparent and widely abused with many Libyans demanding to be sent abroad for treatments that were not necessarily war-related. In January 2012, Libyan deputy prime minister Mustafa Abushagur estimated that $800 million had been spent on this scheme, of which only 15 per cent was actually used by patients who had war-related injuries.
Many hospital directors and senior government figures have been relieved of their duties to make way for candidates deemed more acceptable to the public in a process similar, though not nearly on the same scale as, the de-ba’athification process which occurred in post-2003 Iraq.
As a result, candidates that lack experience and expertise but are deemed to be more acceptable politically are being propelled into leadership positions. Many of these new candidates have achieved revolutionary legitimacy through their actions during the uprising or have been noted for their opposition to the Gaddafi regime whilst in exile.
Furthermore, the present Ministry of Health’s attempts to articulate their policies have been poor as they do not reference any actual policies, preferring instead to tout immeasurable goals such as the “development of all parts of the health system and development of health administration”.
Where do we go now?
A phased approach to rebuilding the capacity of Libya’s public health structures will require technical expertise from international bodies such as the WHO. The already parlous state of human resources in Libya’s health sector (particularly in the areas of health policy, administration and finance) has been exacerbated by constant changes and reshuffles at the ministerial and senior civil service levels.
There is no silver bullet that will solve the Libyan health system’s bureaucratic and management challenges. The best way forward is a holistic, pragmatic and evidence-based approach. To do this, the Ministry of Health first needs to assess the state of Libya’s current healthcare system by conducting a comprehensive Coordinated Needs Assessment. This will allow elected policymakers to make strategic medium and long-term evidence based policy decisions.
Impending elections provide a fresh starting point for an administration to begin, not selected due to ‘revolutionary legitimacy’, but based on their technocratic ability to deliver results in an already beleaguered and struggling sector.
There are many of challenges facing the Libyan healthcare system after such a devastating conflict. However, the current situation represents an unprecedented opportunity to redefine the basis of the entire system. With its strategic location, temperate climate and strong fiscal position, there is no reason why the current trend of medical tourism to Libya’s neighbours should not be reversed. And, with the right policies and adequate technical and financial support, Libya should aspire to being a major healthcare destination itself.
Moez Zeiton is Director for Health Research at the Sadeq Institute, a non-profit, non-governmental think tank based in Libya. This article first appeared in Think Africa Press, www.thinkafricapress.com.
[/restrict]










